Archive for September, 2014
September 27, 2014 at 6:46 pm · Filed under The Restless Legs Diet ·Tagged anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, RLS and Inflammation ·Tagged An ABSOLUTE Cure for RLS, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease
 Unlike drugs, nutrients do not have rapid effects. There’s NO QUICK fix!
Unlike drugs, nutrients do not have rapid effects. There’s NO QUICK fix!
The business of nutrition is to BUILD a better body. That has to wait on Nature to turn over body cells. A blood cell lasts 60 to 120 days. In 3 to 4 months your whole blood supply is completely replaced. In 6 months almost all the proteins in your bones die and are replaced … even the DNA OF YOUR GENES. In a year all your bones and even the enamel of your teeth is replaced.
This time curve is well illustrated by the course of deficiency diseases. If I remove the Vitamin C from your diet, within 4 weeks your blood Vitamin C will drop to zero. But, you will see no symptoms of disease at 4 weeks. You have to WAIT until enough of the HEALTHY cells have been REPLACED by unhealthy cells. It is ANOTHER 12 weeks before the symptoms of scurvy start to ravage your body.
Think of it this way, If you take a neglected house plant and start feeding and watering it, the leaves may PERK UP a BIT from the improved nutrition. But you have to wait for the OLD leaves to die off and NEW leaves to grow before you get a really HEALTHY plant. It is the SAME with the human body. When you start feeding it better, you have to wait on your body to grow NEW improved cells.
To understand the difference between drugs and herbs, let’s focus on how they work. Pharmaceutical drugs are highly purified, potently concentrated chemicals which act by blocking processes of the body. This often gets rid of the symptoms but may create undesired side effects. Anti-congestants will clear your nose, but cause drowsiness. Prolonged use of non-steroids temporarily ease your arthritis pain, but may adversely affect your liver.
 When we drink a tea or take a tincture of an herb, we are taking in the whole plant, with thousands of compounds. Although plants contain unique ingredients which give them specific effects, it is the COMBINATION of all these compounds that accounts for a plant’s effectiveness and safety. The concept that a plant is more than the sum total of all its parts is known as synergy. Synergy means compounds work TOGETHER to boost the power of plants and offset actions of unsafe constituents.
When we drink a tea or take a tincture of an herb, we are taking in the whole plant, with thousands of compounds. Although plants contain unique ingredients which give them specific effects, it is the COMBINATION of all these compounds that accounts for a plant’s effectiveness and safety. The concept that a plant is more than the sum total of all its parts is known as synergy. Synergy means compounds work TOGETHER to boost the power of plants and offset actions of unsafe constituents.
In their wholeness, plants work by effecting favorable changes in our physiology, allowing the body to return to a balanced state. In the holistic tradition, the body knows how to heal itself and will do so given proper assistance. Herbs are our allies in this process.101
In order to get results from herbal treatments it is often necessary to be on a course for several months, especially for serious and/or long-standing problems. Herbs work slowly restoring the body back to balance. There is no magic quick fix with natural medicine because it has to work at such deep levels within the body systems.

SOURCES:
Alternative Medicine for Pets – Nerve damage by Silva Mirovics All Experts en.allexperts.com
How long does it take to heal? by Dr. M. Colgan http://www.diseaseeducation.com
The Whole Herb: Natural Drugs to Help the Body Heal Itself by Mary Jo Ruggieri http://www.columbuspolarity.com
Permalink
September 25, 2014 at 1:54 pm · Filed under ARTICLES by other authors, RLS and Inflammation ·Tagged anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, RLS and Inflammation ·Tagged An ABSOLUTE Cure for RLS, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease
 The cause of disease in our bodies is often silent. It creeps up on us slowly over time, like a smoldering fire that burns unnoticed till one day we wake up with an illness.
The cause of disease in our bodies is often silent. It creeps up on us slowly over time, like a smoldering fire that burns unnoticed till one day we wake up with an illness.
This is true for most chronic diseases like diabetes, high blood pressure, high cholesterol or heart disease. It also true for many other diseases like autoimmune conditions, hormonal imbalances, gastrointestinal diseases, and just about anything that is ends in “itis.”
Medical research has begun to ask questions about what the common underlying causes are of all these problems that create disease in our bodies. And research is looking into what types of tests we can use to find them and measure them.
Chronic inflammation, more accurately known as low-grade or systemic inflammation, is becoming a topic of research to answer questions about the common underlying cause of disease.
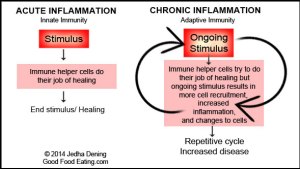
Chronic inflammation is different from the normal or acute, or short-lived, inflammation that occurs when we have a bruise or cut. In acute inflammation our bodies find the bruise or cut, send chemicals into the area, heal the problem, and then our body goes back to its normal processing.
Chronic inflammation is different because the body is not able to shut off the immune response and it continues at a low level, like a fire that is at a smoldering burn for much too long. Over time, this smoldering flame can ignite into a major problem or chronic disease.
This is when you go to the doctor and you are given the diagnoses of diabetes or high cholesterol, when you thought 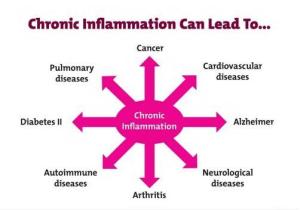 everything was fine. Perhaps you were not feeling well or you have been having symptoms, but you still are surprised by your diagnosis and you don’t know how to solve this unexpected problem.
everything was fine. Perhaps you were not feeling well or you have been having symptoms, but you still are surprised by your diagnosis and you don’t know how to solve this unexpected problem.
There is no standard treatment for chronic inflammation at this time. There does seem to be a benefit to modifying your eating habits toward an anti-inflammatory diet. This would include eating fruits and vegetables, healthy fats, small portions of nuts, eating fish and consuming very little red meat.
One of the markers for chronic inflammation that can be measured by a simple blood test is homocysteine.
This is often measured only in people that have a history or heart disease, but you can request it as part of your normal check up from your doctor.
A normal homocysteine level is found between 4.4 and 10.8 micromoles per liter of blood.
If yours is higher, this can be a marker of inflammation and can contribute to a host of diseases beyond heart disease. There is an increased risk of Alzheimer’s disease for people with high homocysteine levels, as well.
 Living healthy is more than just a cool thing to do. It is a way of life that has positive impact because you don’t end up getting sick over time.
Living healthy is more than just a cool thing to do. It is a way of life that has positive impact because you don’t end up getting sick over time.
Dr. Daemon Jones is a diabetes reversal, hormones, metabolism and weight loss expert. She is a doctor of Naturopathic Medicine based out of the Washington Metropolitan area. http://www.healthydaes.com
Permalink
September 24, 2014 at 1:35 pm · Filed under RLS and Epigenetics ·Tagged anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, RLS and Inflammation ·Tagged An ABSOLUTE Cure for RLS, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease
 There are thousands of articles online about epigenetics. I found this one to be easy to understand, and will help hopefully explain this new breakthrough discovery and why it’s not only important to people suffering from RLS, but for people suffering from any condition.
There are thousands of articles online about epigenetics. I found this one to be easy to understand, and will help hopefully explain this new breakthrough discovery and why it’s not only important to people suffering from RLS, but for people suffering from any condition.
Epigenetics tells us that whatever hand we believe we’ve been dealt … is changeable.
Here’s the article by Marilynn Preston of the Sarasota Herald-Tribune…
The Apple Watch was announced this month with a timeless and bold statement: “Apple Watch is going to greatly improve the way we keep track of our activity and change the way we look at fitness.”
Change the way we look at fitness? Wow, oh wow. Of course I want to write about it instantly, but I can’t because I ended last week’s column with this bit of cleverness: “Come back next week for more happy, hopeful signs that the Healthy Lifestyle Revolution is taking hold and changing our DNA.” I promised. I’m obligated. I feel I must keep my word but now I realize it’s a mistake to end a column with a promise because it keeps me from being seduced by the moment. So epigenetics it is. I’ll write about the Apple Watch next week.
 “Epigenetics … is perhaps the most important discovery in the science of heredity since the gene,” writes David Shenk, author of “The Genius in All of Us: Why Everything You’ve Been Told About Genetics, Talent and IQ Is Wrong.”
“Epigenetics … is perhaps the most important discovery in the science of heredity since the gene,” writes David Shenk, author of “The Genius in All of Us: Why Everything You’ve Been Told About Genetics, Talent and IQ Is Wrong.”
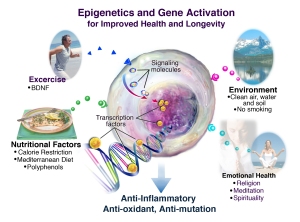
Epigenetics is the next step, the new frontier, the science of changing the way your genes express themselves. Genes can express themselves as disease, or reversal of disease, and the big news is you have much more control over that than you think — if you ever think about your genes at all.
“Basically, epigenetics demonstrates how environment and behavior choices can influence our genetic code,” says Dr. Theri Griego Raby, one of a growing number of doctors who see how epigenetics can play a huge role in disease prevention and well-being.
Contrary to what many of us learned in school, “genes are not fixed predetermined blueprints passed from generation to generation,” Dr. Raby writes, based on the latest epigenetic research.
“Instead, our genome contains at least 4 million ‘switches’ that can be turned on and off by life experiences and 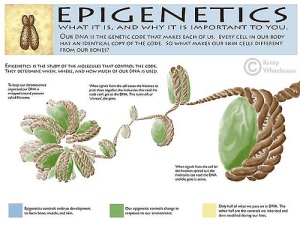 environmental influences.” Life experiences! Environmental influences! That’s where you come in. Scientists now have evidence that lifestyle alone — your choice to smoke, to eat real food, to be physically active — can alter the epigenetic markers that sit above your DNA. The above ones have all the say, not just for your lifetime but affecting future generations.
environmental influences.” Life experiences! Environmental influences! That’s where you come in. Scientists now have evidence that lifestyle alone — your choice to smoke, to eat real food, to be physically active — can alter the epigenetic markers that sit above your DNA. The above ones have all the say, not just for your lifetime but affecting future generations.
I’m wildly oversimplifying, but think about this: Your healthy lifestyle today can predispose your kids and grandkids to greater wellness and a longer life, even before they are conceived! Of course, they then have to make the choices to influence their own genetic code.
It’s fascinating stuff.
So let’s delve a bit deeper.
“Epi” is a prefix that means “above.” Epigenetics looks above the double-helix 25,000-chromosome genetic code and sees another level of influence: the cellular material that sits on top of the genome and outside it.
On top and outside. Get a picture of it. Paint it a color you like.
That “on top” and “outside” cellular material is called the epigenome. Scientists aren’t prepared to say how many epigenome marks there are, but the number is well into the millions. Your genes are your genes, but these epigenetic marks tell your genes to switch on or switch off, to express themselves loudly or go mute.
If you can manage to mute your colon cancer gene, let’s say, by exercising more and eating clean, real food that doesn’t come in plastic, you’re managing your epigenome in a healthy way.
As the biologists like to say, the genome is the hardware, and the epigenome is the software.
And to a large extent, you are the epigenome software programmer in charge. It’s not all fixed and predetermined. Your choices really do matter.
 So what can you do to help your genes behave? Plenty.
So what can you do to help your genes behave? Plenty.
“How we sleep, the types and levels of stress we experience, the type of foods we eat, toxin exposure, alcohol, and lack of exercise can all alter our genetic makeup during gestation, early development, and throughout adulthood,” Dr. Raby says.
“For example, consuming foods rich in gene-altering methyl groups like non-genetically modified soybeans, red grapes, or green tea may protect against disease by deactivating detrimental gene ‘switches.’ ” Enough for today. I welcome you to research more on your own, but know this: Your DNA isn’t your destiny. There is wiggle room, and the sooner you start to shake things up, the better.
Marilynn Preston is a fitness expert, personal trainer and speaker on healthy lifestyle issues. She has a website, marilynnpreston.com, and welcomes reader questions, which can be sent to MyEnergyExpress@aol.com.
Permalink
September 22, 2014 at 12:45 pm · Filed under ARTICLES by other authors, RLS and Inflammation ·Tagged An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease
 AST Enzymes is a leading enzyme manufacturer based in Chino, California. The following article is from their blog …
AST Enzymes is a leading enzyme manufacturer based in Chino, California. The following article is from their blog …
Researchers were initially baffled by patients with restless leg syndrome. Some thought that the disorder could be linked to the nervous system or even caused by a muscular disorder. Restless leg syndrome causes feelings of throbbing, pulling, creeping, unpleasant sensations in the legs that cause an uncontrollable urge to move them. Symptoms primarily occur during the night, and most patients report that moving their legs relieves these symptoms. Doctors were most confused as to why relaxation seems to activate restless leg symptoms. Patients often become frustrated, as sleep cycles are significantly disturbed, affecting quality of life throughout the day.
It’s estimated that 10% of the population suffers from restless leg syndrome, and in most of these cases – the causes remains unknown. Past studies have linked restless leg syndrome to genetic factors, the inability to process a neurotransmitter called dopamine, medications, pregnancy, iron deficiency, and specific chronic diseases.
However, more recent studies seem to focus more on the role of inflammation in restless leg syndrome. There seems to be a pattern, as restless leg syndrome is more common in those with conditions like chronic fatigue, diabetes, and peripheral neuropathy. All of these conditions are related to immune dysfunction caused by inflammation. For this reason, researchers theorized that inflammation may be the trigger in restless leg syndrome.
Once statistical data was gathered, researchers found that there are 38 diseases considered highly related to restless leg syndrome. 95% of these diseases have an inflammatory basis. This suggests that inflammation plays a much larger role in the onset of restless leg syndrome than previously known.
It’s also possible that inflammation can affect other factors that are linked to restless leg syndrome by previous studies. For  example, inflammation is known to trigger iron deficiency – another suspected factor in the onset of this condition. Another focus in restless leg syndrome studies is the microflora in the gut. The gut and its microflora are the nerve center of the immune system, and directly control immune regulation. Imbalanced bacteria levels in the gut may trigger inflammation that can lead to restless leg syndrome.
example, inflammation is known to trigger iron deficiency – another suspected factor in the onset of this condition. Another focus in restless leg syndrome studies is the microflora in the gut. The gut and its microflora are the nerve center of the immune system, and directly control immune regulation. Imbalanced bacteria levels in the gut may trigger inflammation that can lead to restless leg syndrome.
Based on cumulative research and several trigger theories for restless leg syndrome, nutrition should be incorporated in every RLS patient’s regimen. For example, ensuring that iron deficiency is not present is an important preventative strategy. Eating a diet rich in foods known to combat excessive inflammation is also a good idea. Taking natural, anti-inflammatory supplements (not NSAID’s) will help to calm existing inflammation as the beneficial effects of nutrition therapy begin to take effect.
Anti-inflammatory foods include fruits and vegetables that are rich in color. Cherries, peppers, walnuts, fatty fish, berries, beets, tomatoes and dark leafy greens all contain high levels of antioxidants and essential nutrients for immune regulation. Because there is evidence to support the role of inflammation in RLS, controlling systemic inflammation should be of priority as researchers continue to understand this baffling condition. Furthermore, controlling inflammation through the use of natural supplements and nutritional therapy should take precedent over invasive strategies like sedatives or prescription medications that can be habit-forming.
Restless Leg Syndrome – Could Inflammation be to Blame?
Permalink
September 19, 2014 at 1:35 am · Filed under ARTICLES by other authors, RLS and Food Intolerance, RLS and Inflammation ·Tagged An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease
 Irritable Bowel Syndrome (IBS) and Small Intestinal Bacterial Overgrowth (SIBO) are common in RLS.
Irritable Bowel Syndrome (IBS) and Small Intestinal Bacterial Overgrowth (SIBO) are common in RLS.
Three hypotheses developed are
(a) RLS patients are selectively immunocompromised or genetically predisposed and thus more subject to SIBO
(b) SIBO leads to autoimmune changes, and subsequent auto-antibodies attack brain and/or peripheral nerves
(c) SIBO inflammation leads to increased hepcidin and CNS iron deficiency which, in turn, leads to RLS.
These hypotheses bear further investigation.
Gluten Sensitivity, RLS, and SIBO are all Connected…
Research studies have linked gluten ingestion to changes in small intestinal bacteria. These changes can cause a variety of symptoms to occur.
Most commonly patients will experience:
– gas and bloating
– abdominal pain
– intermittent diarrhea and constipation
– acid reflux
– bad breath
Bacterial overgrowth can also lead to changes in digestion, vitamin and mineral absorption, and intestinal permeability (AKA – leaky gut syndrome).
Gluten ingestion can lead to a variety of physiological changes that create disease.
I have treated thousands of patients with gluten issues. Many of them have also had RLS symptoms that resolved on a gluten free diet.
If you haven’t done so already, it is recommended that you get tested for gluten sensitivity or go gluten free.
You can take our self test Here: http://www.glutenfreesociety.org/gluten-free-society-blog/gluten-sensitivity-intolerance-self-test
 Dr. Peter Osborne is the clinical director of Town Center Wellness in Sugar Land, Texas. Dr. is both a doctor of chiropractic as well as a Board Certified doctor of clinical nutrition. He founded the Gluten Free Society in 2010 to help educate patients and physicians on the far reaching effects of gluten sensitivity. He is the author of Glutenology, a series of digital videos and ebooks designed to help educate the world about gluten.
Dr. Peter Osborne is the clinical director of Town Center Wellness in Sugar Land, Texas. Dr. is both a doctor of chiropractic as well as a Board Certified doctor of clinical nutrition. He founded the Gluten Free Society in 2010 to help educate patients and physicians on the far reaching effects of gluten sensitivity. He is the author of Glutenology, a series of digital videos and ebooks designed to help educate the world about gluten.
Permalink
September 10, 2014 at 6:29 pm · Filed under An ABSOLUTE Cure for RLS, ARTICLES by other authors ·Tagged An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease
 Merton came in to my office complaining that he couldn’t sleep. He was tired all day, falling asleep every time he sat down. After some discussion, we found the reason for his sleeplessness: his legs wouldn’t relax, he consistently felt he needed to get up and walk, or move around, all of which is known as Restless Legs Syndrome (RLS).
Merton came in to my office complaining that he couldn’t sleep. He was tired all day, falling asleep every time he sat down. After some discussion, we found the reason for his sleeplessness: his legs wouldn’t relax, he consistently felt he needed to get up and walk, or move around, all of which is known as Restless Legs Syndrome (RLS).
Sometimes, this would wake him up in the middle of the night and he just had to get up and move. The problem had gotten worse since he had quit smoking. When he smoked, he found if he could just take one long drag and hold it in, then the feeling would go away.
We tried many remedies, including sleeping pills and natural sedatives, but nothing worked. I was ready to throw in the towel and tell him to take up smoking again, until I thought that his problem might be related to something in the tobacco – nicotine! Nicotine in tobacco can increase dopamine in the brain and “treat” some people with RLS.
Restless leg syndrome is not a disease; it’s merely a symptom. There are multiple reasons for having this problem so there isn’t one cure for people with RLS. Since most RLS seems to be an imbalance of dopamine in the brain, it has been treated as Parkinson’s disease with dopamine-like drugs such as L-dopa or Requip. The problem with these is that they cause inflammation in the part of the brain that produces dopamine and, over time, can make the problem worse. Before you consult a medical specialist I would recommend trying the following, one at a time:
Proper Avoidance
First of all you should avoid stimulants such as sugar (yes, it’s a stimulant), MSG and caffeine. Especially avoid energy drinks.
Mineral balance
The ability for muscles to relax requires a proper balance of sodium and potassium, as well as calcium and magnesium.
Mostly, we get enough sodium and calcium, but not enough potassium and magnesium. These can be taken as supplements, but I always recommend using foods first.
 The foods that contain both of these are:
The foods that contain both of these are:
•Green vegetables
Many are amazed at how their restlessness disappears when the eat greens as a significant proportion of their diet.
•Fruit
You have probably heard that bananas contain lots of potassium, and they do, but most other fruit does as well.
•Nuts and seeds
These are best eaten fresh a nd raw so the oils aren’t oxidized.
•Whole grains
When grain is processed, the magnesium is removed. I recommend avoiding all processed grains for many other reasons also.
Supplements that I have seen work in the past include:
• magnesium powder
• calcium lactate 400mg at night
• potassium iodide 40mg with a meal
Vitamins E and F
The modern diet has a tremendous imbalance of oils. Those with Restless Leg Syndrome have significantly lower levels of essential oils and vitamin E.
Vitamin F is the name given to all the 5 essential fats that our bodies can’t make – we need to eat them. One of the functions of these fats is to regulate the absorption and utilization of minerals such as calcium. This is the
RLS connection. This regulation allows the muscles to relax normally.
Recommendations: Eat fish or flax seeds or take flaxseed oil or fish oil 5 grams per day. Take “Mixed Tocopherols” or natural vitamin E 600 IU per day.
 Niacinamide and L-Tryptophan
Niacinamide and L-Tryptophan
Vitamin B3 is an important part of energy production. Moreover, having this vitamin in sufficient amounts is important for the production of Serotonin, which is made from L-Tryptophan and has a calming effect on the brain.
Recommendations: Niacinamide, 500mg three times per day with meals and L-Tryptophan 2000mg at night on an empty stomach.
Folic Acid
If RLS runs in your family, it might be because of a relative folic acid deficiency. Some people don’t “methylate” folic acid very well. Even though their blood levels are normal, they can’t use it properly. Those with
this problem may need up to 30mg of folic acid per day.
Recommendation: You must use the amount required to relieve the symptoms, adjusting the dose as needed. You may also find that you need considerably less if you get the activated form, called MTHF (methytetrahydrofolate or methylfolate).
Iron
Studies indicate iron to be a major player in RLS because it is needed to make dopamine. Most people who suffer from RLS either have low total body iron, or just in the brain. Be careful with iron supplementation because too much iron causes inflammation. Ideally, you would want a test of iron levels before taking extra.
Recommendation: Supplement iron with an iron nail (16-penny NOT galvanized) clean it off with sandpaper or steel wool and put it into an orange. The next day take it out and eat the orange. Put the nail in the next orange. The following day take the nail out and eat the orange, putting the nail into another orange. Continue with this daily. Within one week you should have noticeable improvement. If not, you probably don’t need iron.
There isn’t just one “cure” for Restless Leg Syndrome. Merton finally found relief when we increased his dopamine levels and slept like a baby.
If you feel like you need to move your legs you might consider the above natural treatments: calcium, magnesium, potassium, iron, folic acid and vitamin E.
It may take some trial-and-error, but it’s worth avoiding drugs and getting a good night sleep.
 Dr. Scott D. Saunders, MD is a practicing physician, specializing in preventative healthcare, who utilizes eclectic health care for the whole family, including conventional, orthomolecular and natural medicine. He is also the medical director of The Integrative Medical Center of Santa Barbara in Lompoc, CA. He went to UCLA medical school and is board certified in family medicine.
Dr. Scott D. Saunders, MD is a practicing physician, specializing in preventative healthcare, who utilizes eclectic health care for the whole family, including conventional, orthomolecular and natural medicine. He is also the medical director of The Integrative Medical Center of Santa Barbara in Lompoc, CA. He went to UCLA medical school and is board certified in family medicine.
Permalink
September 7, 2014 at 8:26 pm · Filed under Scientific Studies Linking RLS and Inflammation ·Tagged An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease, willis-ekbom remedy
 This article is based on a lecture from the XLVII European Renal Association-European Dialysis and Transplant Association Congress.
This article is based on a lecture from the XLVII European Renal Association-European Dialysis and Transplant Association Congress.
Giulio Romano, MD, professor of nephrology at the University of Udine in Italy, told Medscape Medical News that “the interesting conclusion of our work is that there is a correlation between Restless Legs Syndrome and an increase of inflammatory cytokines and the increase of CRP (inflammation biomarker).”
Dr. Romano noted that several studies have shown that increased inflammation is associated with elevated cardiovascular risk in patients on chronic hemodialysis. Also, he said there is evidence that sleep disorders induce elevated levels of proinflammatory cytokines.
“We think that if patients have some sleep disorders, they evoke inflammation,” he said; “if we treat the sleep disorders, we reduce a cardiovascular risk factor because CRP is a possible cause of increased cardiovascular risk.” The hemodialysis patients without RLS, he noted, had much lower CRP levels. Similarly, the levels of transferrin saturation, another marker of inflammation, were different between patients with and without RLS.
 Nageswara Reddy, MD, assistant professor of nephrology at Manipal University in India, who was not involved with the study, told Medscape Medical News that it makes sense to him that RLS is associated with inflammatory markers. Cardiovascular mortality, which is the main cause of death among hemodialysis patients, is associated with elevated levels of CRP, but it might be associated with other underlying causes as well.
Nageswara Reddy, MD, assistant professor of nephrology at Manipal University in India, who was not involved with the study, told Medscape Medical News that it makes sense to him that RLS is associated with inflammatory markers. Cardiovascular mortality, which is the main cause of death among hemodialysis patients, is associated with elevated levels of CRP, but it might be associated with other underlying causes as well.
“We have to find out all risk factors. Maybe lack of sleep is another risk factor,” Dr. Reddy hypothesized, and suggested that other inflammatory markers, in addition to CRP, be investigated.
You can read the full article here:
http://www.medscape.com/viewarticle/724535
Permalink
September 6, 2014 at 6:03 pm · Filed under RLS.org ·Tagged An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease, willis-ekbom remedy
 All this crazy talk about non medical cures for RLS has got me banned from RLS.org again. This time I suspect for good.
All this crazy talk about non medical cures for RLS has got me banned from RLS.org again. This time I suspect for good.
It really is a crime that an organization that gathers people together in a unified search for a solution, would ban someone that offers proof that there are solutions.
They are so tightly bound to the pharmaceutical industry, it’s frightening.
I realize that they’re no different than any other foundation, it’s just that I’m seeing one up close for the first time.
I’m mostly frustrated because they’re misleading thousands of people, saying that their only chance at relief is through medication.
These are people that trust that they are being told the truth, and they’re not.
They’re being horribly misled.
Permalink
September 5, 2014 at 6:28 pm · Filed under An ABSOLUTE Cure for RLS ·Tagged An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease, willis-ekbom remedy
 THE NOETIC SCIENCES SPONTANEOUS REMISSION PROJECT
THE NOETIC SCIENCES SPONTANEOUS REMISSION PROJECT
Hopefully those of you that are stuck in a deep, seemingly hopeless pit with your RLS, can draw some inspiration from this study.
In 1993, the Institute of Noetic Sciences published “Spontaneous Remission: An Annotated Bibliography.”
In this work, the authors defined spontaneous remission as “the disappearance, complete or incomplete, of a disease or cancer without medical treatment or treatment that is considered inadequate to produce the resulting disappearance of disease symptoms or tumor.”
From their website:
http://www.noetic.org/research/project/spontaneous-remission
“The Remission Project catalogued the world’s medical literature on the subject and the resulting book was the largest database of MEDICALLY REPORTED cases of spontaneous remission in the world, with more than 3,500 references from more than 800 journals in 20 different languages.
An example of “pure remission” would be a patient diagnosed with bone cancer, who refused treatment and who is disease-free more than 10 years later (so we’re not talking about the placebo effect).
Spontaneous remission of cancer has been reported in almost every type of cancer. The largest number of cases are reported in a few types of cancer: neuroblastoma, renal cell carcinoma, melanoma, and leukemias/lymphomas comprise the largest number of cases reported.
Psychological and spiritual factors play a role in remission and survival is evident from the stories of people who have experienced unexplained recoveries from cancer and other diseases, but since the role of mind and the spirit is different for each person, it is difficult to generalize their influence.”
SO, WHAT DOES THIS HAVE TO DO WITH RESTLESS LEGS SYNDROME?
Even though there is “no cure” for cancer, thousands of people over the years have beat the disease.
And there is no set way to this “cure.” There’s no pattern. They all had to do it in a way that WORKED FOR THEM.
Through a combination of a focused determination, perseverance, courage, changes in diet, beliefs & attitudes, physical exercise, meditation, prayer etc. they beat an unbeatable disease.
They overcame their cancer by creating a cure through trial and error, based on their own life experience, using the successes of others as a “guideline.”
 “THERE IS NO CURE FOR RESTLESS LEGS SYNDROME!!!!!!“
“THERE IS NO CURE FOR RESTLESS LEGS SYNDROME!!!!!!“
Yes, I’ve heard it a million times.
For several years now I’ve posted on RLS community boards information that I believe would be helpful to those that are suffering.
The most common reaction I get is that there is “NO CURE FOR RLS!” (followed by YOU QUACK, YOU FRAUD, YOU DISGUSTING EVIL PERSON etc.).
In fact the reaction is so strong I’ve been banned for good from RLS.uk. And on top of that, no current member is even allowed to reference me or my website.
I was banned from both RLS.org and RLS.org.au but was allowed back to both. I know I’m currently on thin ice on one of them. I’m on thin ice, and I censor myself so intensely it’s embarrassing, just to avoid getting the boot again.
One nutcase that runs a Yahoo RLS group notified the FDA about me.
All because I claim there is a cure.
I guess if you can invoke that type of reaction you must be doing something right?
It is criminal that these so called “moderators” screen out the information just because they disagree with it – information that the new or casual observer is unable to read and decide for his or herself whether or not they would like to follow up on it.
I understand that in their minds, the moderators are protecting their flock, but the truth is they have serious control issues that are condemning their members to “life on meds” – continually brainwashing them with the idea that THERE IS NO CURE.
“Stay on your meds and wait with the rest of us for a cure!”
That’s the message.
THE DEFINITION OF INCURABLE
Here is the definition of Incurable from Dictionary.com
adjective
1. not curable; that cannot be cured, remedied, or corrected:
an incurable disease.
2. not susceptible to change.
So, by definition, since I had RLS and no longer have it (and many others as well) that means RLS is actually NOT incurable. It is then by definition, curable.
 WHY ARE ALL THE SUCCESS STORIES IGNORED?
WHY ARE ALL THE SUCCESS STORIES IGNORED?
There are hundreds, probably thousands of people that suffered from RLS, and because of changes in their life, no longer do.
Yet the most common response I get to my claim is not “what did you do to break free, for God’s sake, please tell me!”
The most common response is “you didn’t really have it” or even better “you’re just making this all up!”
It sounds like a really bad parent, doesn’t it?
Of course the claim of these hardliners (and there are many of them) is that their RLS is REALLY REALLY REALLY BAD … something the average sufferer couldn’t even imagine, or endure.
It’s only the people with mild or pretend RLS that get better.
It’s the heroic ones that still suffer with the “TRUE” RLS.
PEOPLE TAKE IT PERSONALLY
When I post something that hints that there is a cure for RLS, people start freaking at me, interpreting my post as an attack on their character.
They feel that I’m telling them that because they are on meds, they are weak.
Nothing could be further from the truth.
The reason I post the information is so that people who are trapped in a living Hell can “consider” alternatives. I’m only trying to let them know that there are options.
If you escaped from something that was inescapable, would you not try to help others who are still trapped?
It’s human nature.
The whole foundation of self-help groups is based upon this principle.
 YOU CAN STAY ON MEDS AND DEVELOP A PLAN OF ACTION
YOU CAN STAY ON MEDS AND DEVELOP A PLAN OF ACTION
My wife Barb developed a three year multi-stage plan to quit smoking. I had to respect that. That’s what SHE needed to do in order to quit. She developed a plan of action based on HER life experience and HER character and set it in motion.
And it worked. At the end of the process she stopped smoking. She hasn’t had a cigarette in eight years.
However, if she was to push her method on a friend who still smoked, it would be violently rejected.
Her friend has to develop her OWN plan of action.
Her friend, when she decides to quit, can reference what has worked for other people, but for her to succeed, it has to be done HER way, on HER terms.
The cure for RLS is no different.
“I TRIED EVERYTHING AND IT DIDN’T WORK!!!”
The most common excuse is “There is no cure because I tried everything and it didn’t work!”
That’s like saying “I TRIED AA AND IT DOESN’T WORK … SO I HAVE NO CHOICE BUT TO CONTINUE DRINKING!”
I know from several people that I’ve talked to that they have dramatically changed their diet. Yet, they still suffer.
It doesn’t mean that there isn’t a solution for them. All it means is that they haven’t found it yet.
Every “cure” is going to be a bit different for each person. Just like with spontaneous remission and my wife’s smoking.
But, there IS a cure that exists for every one of you reading this.
It all comes down to how much effort are you willing to put into finding it? And are you willing to change your actions, beliefs and attitudes?
SO WHO IS THIS “EXPERT” THAT SAYS THERE IS NO CURE?
Who is this mystery person that originally informed the world that there is no cure for Restless Legs Syndrome?
Maybe it’s Dr. Mark Buchfuhrer, the legendary RLS specialist “Dr. B” that used to be in a Mirapex commercial?
It can’t be any of the doctors that I’ve quoted from articles and studies. They’re all quacks.
Regardless of who the source is, I’ve never been shown one solid piece of evidence showing that RLS is not curable. In fact it’s quite the opposite.
It’s always just a knee-jerk reaction, with no evidence to support the “incurable” claim.
It’s kind of like atheists continually asking people to prove there is a God. Yet, they’ve never offered one grain of evidence proving there isn’t.
MY SMALL BUT GROWING DATABASE OF SUCCESS STORIES
The truth is more and more people are taking the situation into their own hands and are making the necessary changes to become free of there RLS.
You can read about several of them here: http://www.rlcure.com
 IN CLOSING
IN CLOSING
Let’s face it, what people really mean when they say there is no cure for RLS, is that there is no DRUG that will take it away.
All the successes that happen to the flaky people are anecdotal. There’s no substance to any of it.
For those of you suffering from RLS, I wish you the very best.
I sincerely hope that you can draw some inspiration from the Spontaneous Remission Project.
You can read it online here:
http://www.noetic.org/library/publication-books/spontaneous-remission-annotated-bibliography
Permalink
September 4, 2014 at 2:43 pm · Filed under RLS Success Stories ·Tagged An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease, willis-ekbom remedy
 “I was diagnosed with RLS about sixteen years ago. My symptoms were primarily showing themselves in the evening, making it difficult to sit and watch TV, go to a concert, etc, let alone go to bed and sleep.
“I was diagnosed with RLS about sixteen years ago. My symptoms were primarily showing themselves in the evening, making it difficult to sit and watch TV, go to a concert, etc, let alone go to bed and sleep.
I had tried lots of drugstore sleep remedies with little relief before being diagnosed.
After the diagnosis, I started on Requip, which really gave me a lot of symptom relief. Problem was, I was almost unable to stay awake during the evening, long before wanting to go to bed for the night. Also, while the legs were quieted, I found myself still restless and irritable, so after awhile, I was switched to Mirapex. Things were somewhat better for awhile, until augmentation began.
Symptoms began earlier in the day, and required more drug to suppress them, so that I would zonk out when the symptoms let up. I read enough information to realize that this class of drugs would probably have to be abandoned soon, leaving others that would be very sedating, as well. Kind of a depressing outlook, since I don’t really aspire to die in the next few years.
On day my daughter sent me a website http://www.rlcure.com that talked about natural remedies for RLS (this was after yet another conversation with me about how bummed I was about this miserable ailment and wondering what shape I’d be in in the coming years).
As a very experienced RN, and a natural skeptic besides, my first thought was “Oh, RiGHT!”, and after reading a little on the site, I thought, “How can I do all that?” Yet, as a nurse, it did make some sense to me. I already knew about the evidence showing that inflammation plays a role in a lot of medical conditions, so was it really so far-fetched to see it as a factor in RLS? Then there was the question my husband posed…”Wouldn’t you do almost anything to get rid of that?”
I started with cayenne (which I stopped because of frequent stomach upset) and Curcamin which is a combo drug available at some natural or organic stores as well as via Amazon. I am sorry to say that I don’t know for certain what the third one was that I took, but I can tell you that magnesium, calcium, B-12 sublingual, B complex and Quercitin with Bromelain (also found at natural stores or Amazon) were added soon, and help me a lot.
I also drink carrot juice. Of course, everyone has their own scenario of symptoms. There is also a large list of supplements in which to choose, but I have stuck with these.
I also occasionally use L-theanine to help settle me when I am especially bothered. It’s very mild, just calming.
After only a few weeks, I was able to decrease my Mirapex by half.
The dietary changes are harder, but when I follow them, my evenings are better.
Since they are mostly principles I should follow for glucose and weight control as well, I am working on better compliance, and truly believe I may be able to be prescription – free in time. And even if I don’t get that far, I am in a much better situation and feel much less helpless because of the anti-inflammatory approach.
It is a great feeling to believe you can be proactive in dealing with this illness!! I have passed along some of this to others, and highly recommend trying this method to anyone living with this nasty condition….”Wouldn’t you do almost anything to get rid of that?”
About me: I am 66yrs. old, lived all my life in Wisconsin. Have been married for 44 yrs, and worked for 43 yrs as an RN, most of it in hospital nursing, with many years in cardiology and cardiac surgery. We have an adult son and daughter, a grandson who is 5 yrs, old, and will be excited to welcome a granddaughter in October. We also love our pets, traveling, and music. We enjoy a wonderful Christian church. We are becoming more health-conscious as we get older, and really hope to be active “senior citizens”! having my RLS under control will be important for that.
_______________________________________________
For more RLS success stories visit http://www.rlcure.com
If you have a success story, please e-mail me at dwimble@magma.ca
Permalink
September 1, 2014 at 8:11 pm · Filed under RLS and Inflammation, Scientific Studies Linking RLS and Inflammation ·Tagged alternative medicine, An ABSOLUTE Cure for RLS, anti-inflammatories, anti-inflammatory, aspartame, astaxanthin, caffeine, calcium, cayanne, chronic inflammation, curcumin, David Wimble, diet, dopamine, dopamine levels, Dr. Leonard Weinstock, Electromagnetic Fields, EMF, epigenetics, epigenome, ferritin, ferritin level, flora, food intolerance, gaba, ginger, glutamate, glutamine, gluten, Gut Microbiota, herbal remedies, herbs, Histamine Intolerance, histamines, homeopathy, inflammation, Inflammation and RLS, inflammation remedies, insomnia, iron, iron level, leaky gut, magnesium, microbiome, minerals, monosodium glutamate, msg, natural antihistamines, natural healing, natural medicine, nsaids, nutrution, omega 3, probiotics, restless arms, restless feet, restless leg syndrome, Restless Legs and Insomnia, restless legs cure, restless legs remedy, restless legs symptoms, restless legs syndrome, restless legs syndrome symptoms, rls, RLS and Epigenetics, RLS and Food Intolerance, RLS and Inflammation, rls cure, rls remedy, rls symptoms, salt, silent inflammation, sleep disorders, st. john's wort, sugar, systemic enyzmes, The Restless Legs Diet, vitamin b12, vitamin c, WED, willis-ekbom, willis-ekbom cure, willis-ekbom disease, willis-ekbom remedy
 MYTH #1: RLS IS GENETIC
MYTH #1: RLS IS GENETIC
TRUTH: The “tendencies” that cause RLS are passed down from parent to child. These tendencies are VERY changeable. They are not hard-coded.
Epigenetics are the switches that turn these tendencies OFF or ON.
Science now knows with absolute certainty that genetics play a much smaller role than previously thought.
Here’s a quote from Newsweek Magazine about the new exciting world of epigenetics.
“Roll over, Mendel. Watson and Crick. They are so your old man’s version of DNA. And that big multibillion-dollar hullabaloo called the Human Genome Project? To some scientists, it’s beginning to look like an expensive genetic floor pad for a much more intricate – and dynamic – tapestry of life that lies on top of it.” – Newsweek Magazine, June 2009
Genetics determine certain traits that are passed on to children, such as hair color, the shape of the nose etc. (as we all learned in school) but beliefs, tendencies and conditions that are passed on are passed through what is called “epigenetics.” These are the switches that determine how our genes are going to act.
For instance, if a parent was extremely negative, those negative switches would be already turned on in the child’s genetic makeup, even before it was born. The child would have to take an action to change the switches to turn the positive genes on and the negative genes off.
In the case of RLS, the bad switches could be on because of diet, environment, and in a lot of cases, stress. This would create inflammation in the parent, and at some point in the child’s life, sometimes very early. These switches would cause inflammation to build until actions were taken and changes were made.
Here’s a quote from a 2012 study:
“Phenocopies in families with essential tremor and restless legs syndrome challenge Mendelian laws. Epigenetics might provide answers.” Zimprich A. Parkinsonism Relat Disord. 2012 Jul;18(6):711-6.
“There is increasing evidence that epigenetic modifications, which refer to changes in gene expression without changes in DNA sequence, can be transmitted to the next generation. Moreover, epigenetic information can be transferred from one allele of a gene to the other allele of the same gene; if then inherited to the next generation, the offspring consequently presents phenotypic properties related to the untransmitted allele.”
Note that if a parent had inflammatory tendencies in the way they lived their life, the inflammation could eventually manifest in the child in a number of ways. It could become RLS as well as hundreds of other inflammatory conditions including depression, ADHD, Parkinson’s etc.
For an extensive look at epigenetics visit:
http://www.rlcure.com/epigenetics-and-restless-legs-syndrome.html
 MYTH #2: THERE ARE “TWO” TYPES OF RLS – PRIMARY AND SECONDARY
MYTH #2: THERE ARE “TWO” TYPES OF RLS – PRIMARY AND SECONDARY
TRUTH: There is only ONE type of RLS. RLS is ALWAYS caused by inflammation, not by another condition.
Having chronic inflammation in your body is like spilling a coffee on your keyboard. Something unpleasant is going to happen, you’re just not sure what.
In the now famous 2012 study by Dr. Leonard Weinstock titled “Restless Legs Syndrome: Theoretical Roles of Inflammatory and Immune Mechanisms” it was shown that 36 of the 41 RLS-associated conditions (88%) have been associated with inflammatory and/or immune changes.
According to the study “The fact that the majority of highly RLS associated conditions are also associated with inflammatory/immune changes suggests the possibility that RLS may be mediated or affected through these mechanisms.”
Parkinson’s, IBS, SIBO, Cancer or any of the other secondary conditions the study refers to do not cause RLS. Inflammation is causing BOTH of the conditions.
Keep in mind that inflammation can manifest as one condition, two conditions or more if it’s not addressed.
You can read about the study at the website below, which also includes some additional data that shows why the results should have shown that 100% of the conditions are associated with inflammation.
http://www.rlcure.com/scientific-study-suggests-inflammation-is-a-primary-cause-of-RLS.html
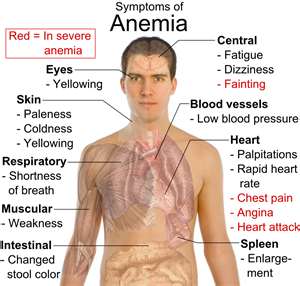 MYTH #3: IRON DEFICIENCY IS A PRIMARY CAUSE OF RLS
MYTH #3: IRON DEFICIENCY IS A PRIMARY CAUSE OF RLS
TRUTH: The inflammation causing the RLS also affects iron levels.
The medical text “Hyperkinetic Movement Disorders: Differential Diagnosis and Treatment” by Alberto Albanese and Joseph Jankovic (John Wiley & Sons, 2012) is a scholarly work written for pediatric and adult endocrinologists, orthopaedic surgeons, roentgenologists, workers in rheumatology clinics, geneticists, nutritionists and very specialized osteologists. The book is a collection of data and observations made through a variety of scientific studies.
Chapter 20 of the book focuses on Restless Legs Syndrome. On page 311, Arthur S. Walters M.D. of the Vanderbilt Department of Neurology is quoted.
“Most recently we have noted that RLS patients have an increased prevalence of Irritable Bowel Syndrome (IBS) and an increased prevalence of Small Intestinal Bacterial Overgrowth (SIBO) compared to controls. This led us to review the 40 or so secondary causes of RLS. Independent of RLS, the vast majority of these secondary causes are associated with either iron deficiency, SIBO or inflammatory/immune abnormalities.
This suggests that inflammation and immune attacks on the peripheral or central nervous system in RLS could be pathogenetic to RLS.
An alternative explanation is that inflammation may lead to iron deficiency which may in turn lead to RLS.”
It is well known in the scientific community that inflammation can affect iron levels. Below are a couple of studies that support this idea:
“Influence of acute inflammation on iron and nutritional status indexes in older inpatients.” MM Chiari et al. J Am Geriatr Soc. 1995 Jul;43(7):767-71.
“Patients with acute inflammation present altered iron status indexes that resemble those observed in the anemia of chronic disease.”
“Interpretation of biochemical tests for iron deficiency: diagnostic difficulties related to limitations of individual tests.” Frank Firkin, Director of Clinical Haematology; and Bryan Rush, Director of Laboratory Haematology, St Vincent’s Hospital, Melbourne.
“Most cases of iron deficiency can be diagnosed with simple tests. The concentration of serum iron does not fall until the body’s iron stores are exhausted. As the stores are depleted, the concentration of transferrin rises while the concentration of ferritin falls.
Caution is required when assessing patients with inflammatory disease as a low serum iron may not represent iron deficiency. These patients often have reduced concentrations of transferrin.”
MYTH #4: RLS IS CAUSED BY AN IMBALANCE OF DOPAMINE LEVELS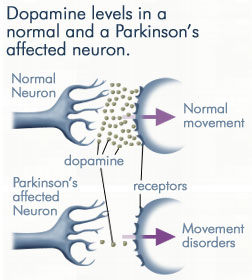
TRUTH: The dopamine imbalance and the Restless Legs are BOTH caused by INFLAMMATION.
A dopamine imbalance can be caused by low iron levels or directly from inflammation as is stated in the following studies:
“CSF iron, ferritin and transferrin levels in restless legs syndrome.” Soichi Mizuno et al. Department of Psychiatry, Shimane University School of Medicine, Shimane, Japan, February 2004.
“The results of this MRI study suggest that idiopathic RLS patients may have a dysfunction of dopamine production induced by the iron deficiency in a dopamine-related specific area of the brain, and support the iron-dopamine model of this syndrome.
“Iron deficiency alters expression of dopamine-related genes in the ventral midbrain in mice” L.C. Jellena et al. Neuroscience, Volume 252, 12 November 2013, Pages 13–23
“A clear link exists between iron deficiency (ID) and nigrostriatal dopamine malfunction. This link appears to play an important role in at least restless legs syndrome (RLS) if not several other neurological diseases.”
“Iron deficiency alters dopamine uptake and response to L-DOPA injection in Sprague–Dawley rats.” Laura E. Bianco1 et al. Journal of Neurochemistry, Volume 106, Issue 1, pages 205–215, July 2008.
“Iron deficiency (ID) disrupts brain dopamine (DA) and norepinephrine (NE) metabolism including functioning of monoamine transporters and receptors.”
“Inflammation induces mitochondrial dysfunction and dopaminergic neurodegeneration in the nigrostriatal system.” RL Hunter et al. Journal of Neurochemistry. 2007 Mar;100(5):1375-86.
“Evidence suggests that chronic inflammation, mitochondrial dysfunction, and oxidative stress play significant and perhaps synergistic roles in Parkinson’s disease (PD), where the primary pathology is significant loss of the dopaminergic neurons in the substantia nigra.”
“Systemic Infusion of Naloxone Reduces Degeneration of Rat Substantia Nigral Dopaminergic Neurons Induced by Intranigral Injection of Lipopolysaccharide.” Bin Liu et al. The Journal of Pharmcology and Experimental Therapeutics Vol. 295, No. 1, JPET 295:125-132, (2000).
“A massive degeneration of dopamine-containing neurons in the substantia nigra (SN) in the midbrain is characteristic of Parkinson’s disease. Inflammation in the brain has long been speculated to play a role in the pathogenesis of this neurological disorder.”
 MYTH #5: RESTLESS LEGS SYNDROME IS A DISEASE
MYTH #5: RESTLESS LEGS SYNDROME IS A DISEASE
TRUTH: RLS is a BIOMARKER indicating that your body is dangerously INFLAMED and that ACTIONS must be taken to prevent further damage.
RLS is now officially Willis-Ekbom Disease (WED). The name change occurred a few years ago to give it more credibility, but the truth is it’s an uninspiring name and is rarely used by anyone outside of RLS.org.
The body is an incredibly complex machine and one of its survival mechanisms is its ability to send our warning signals when something is not right underneath the hood.
For example, frequent headaches indicate that something beneath the surface needs to be attended to, whether it be stress, lifestyle, a tumor, inflammation or something else.
In the case of RLS, your body is telling you that you have too much inflammation and that it must be dealt with. If no changes are made, the inflammation will increase and lead to additional conditions.
A nationally-recognized sleep expert has published an editorial describing Restless Legs Syndrome (RLS) as a possible biomarker for underlying disease. The editorial appears in the March 5, 2014 issue of Neurology the medical journal of the American Academy of Neurology and was authored by Boston Medical Center neurologist Sanford H. Auerbach, MD.
Auerbach suggests that restless leg syndrome is a meaningful biomarker for serious disease, and that RLS screening may become more common as a tool for primary care providers to identify patients at risk.
Find out more here:
http://medicalxpress.com/news/2014-03-restless-legs-syndrome-signify-bigger.html
http://www.rlcure.com/restless-legs-syndrome-willis-ekbom-is-not-a-disease.html
MYTH #6: RLS IS OFTEN CAUSED BY PREGNANCY
TRUTH: The RLS is caused by the HIGHER presence of INFLAMMATION in pregnant women.
As the studies below demonstrate, inflammation levels tend to increase in pregnant women.
“Vaginal cytokines in normal pregnancy.” G. Gilbert et al. American Journal of Obstetrics and Gynecology, vol. 189, no. 5, pp. 1433–1438, 2003.
“A significant increase of proinflammatory cytokines (IL-6 and IL-8) is produced in the third trimester. These cytokines act as chemoattractants of polymorphonuclear leukocytes stimulating the expression of prostaglandins in response to delivery preparation.”
“C Reactive Protein levels are elevated in the Third Trimester in Preeclamptic pregnant Women.” Zaima Ali et al. Dept. of Physiology, Lahore Medical and Dental College, Department of Obstetrics and Gynecology, Jinnah Hospital, Lahore.
“Pregnancy is a complex process which leads to a number of systemic changes. During normal pregnancy all these changes are very well regulated. Preeclampsia is a very common disorder of pregnancy and is characterized by hypertension and proteinuria that begins at more than 20 weeks of gestation. Poor placentation with inadequate cytotrophoblast invasion results in widespread maternal endothelial dysfunction. There is increasing evidence that preeclampsia is accompanied by exaggerated maternal systemic inflammatory response to this poor placentation.”
“Prokineticin-1: A Novel Mediator of the Inflammatory Response in Third-Trimester Human Placenta.“ Fiona C. Denison et al. Endocrinology. 2008 July; 149(7): 3470–3477. doi: 10.1210/en.2007-1695
“Prokineticin-1 (PK1) is a recently described protein with a wide range of functions, including tissue-specific angiogenesis, modulation of inflammatory responses, and regulation of hemopoiesis. The aim of this study was to investigate the localization and expression of PK1 and PK receptor-1 (PKR1), their signaling pathways, and the effect of PK1 on expression of the inflammatory mediators cyclooxygenase (COX)-2 and IL-8 in third-trimester placenta.
Our study demonstrates that PK1 and PKR1 are highly expressed in third-trimester placenta with PK1 up-regulating expression of IL-8 and COX-2 potentially via activation of PKR1 and cross-talk with EGFR. The latter finding is supported by double-immunofluorescent immunohistochemistry studies that show that PKR1 colocalizes with IL-8 and COX-2 in placenta. Together, these data suggest that PK1 may be a novel paracrine mediator of the inflammatory response in third-trimester placenta.”
 MYTH #7: AGING TENDS TO CAUSE RLS
MYTH #7: AGING TENDS TO CAUSE RLS
TRUTH: The RLS is caused by the HIGHER presence of INFLAMMATION in elderly people.
As the studies below demonstrate, inflammation levels tend to be higher in the elderly population.
“Inflammation in aging: cause, effect, or both?” NS Jenny. Discov Med. 2012 Jun;13(73):451-60.
“Aging is a progressive degenerative process tightly integrated with inflammation.”
“Chronic Low-Grade Inflammation in Elderly Persons Is Associated with Altered Tryptophan and Tyrosine Metabolism: Role in Neuropsychiatric Symptoms.” L. Capuron et al. Biol Psychiatry. 2011 Jan 28.
“Our findings show that chronic low-grade inflammation in aging is associated with alterations in enzymatic pathways involved in monoamine metabolism and suggest that these alterations might participate in the pathophysiology of neuropsychiatric symptoms in elderly persons.”
“Age-related alterations in retinal neurovascular and inflammatory transcripts.” CA Van Kirk et al. Mol Vis. 2011;17:1261-74.
“The commonalities in retinal age-related and diabetes-induced molecular alterations provide support for the hypothesis that diabetes and aging engage some common para-inflammatory processes.”
Permalink
 Unlike drugs, nutrients do not have rapid effects. There’s NO QUICK fix!
Unlike drugs, nutrients do not have rapid effects. There’s NO QUICK fix!
 When we drink a tea or take a tincture of an herb, we are taking in the whole plant, with thousands of compounds. Although plants contain unique ingredients which give them specific effects, it is the COMBINATION of all these compounds that accounts for a plant’s effectiveness and safety. The concept that a plant is more than the sum total of all its parts is known as synergy. Synergy means compounds work TOGETHER to boost the power of plants and offset actions of unsafe constituents.
When we drink a tea or take a tincture of an herb, we are taking in the whole plant, with thousands of compounds. Although plants contain unique ingredients which give them specific effects, it is the COMBINATION of all these compounds that accounts for a plant’s effectiveness and safety. The concept that a plant is more than the sum total of all its parts is known as synergy. Synergy means compounds work TOGETHER to boost the power of plants and offset actions of unsafe constituents.




































